When it comes to ectopic pregnancy, I believe everyone will not be too unfamiliar, but the understanding is only limited to the extent of its harm. In fact, understanding the causes of ectopic pregnancy, whether for the treatment of this situation, or for the prevention of ectopic pregnancy, are of great help, so what causes ectopic pregnancy do you know what? The following is a summary of the main causes of ectopic pregnancy.
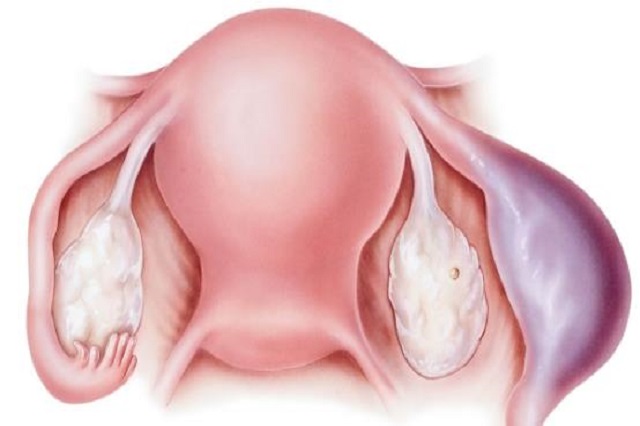
What reason can cause ectopic pregnancy?
1. Salpingitis: tubal inflammation is one of the main causes of ectopic pregnancy. Clinically, the disease can be divided into tubal mucositis and salpingitis. Therefore, it is necessary to treat this disease in time.
2. Have ectopic pregnancy history: tubal pregnancy history will also increase the risk of ectopic pregnancy again. For example, women who have suffered from tubal pregnancy must pay attention to the investigation when they are pregnant again.
3. Intrauterine device contraceptive failure: the placement of intrauterine device may also cause ectopic pregnancy. For example, if women because of contraceptive contraceptive failure and pregnancy, it will create favorable conditions for the occurrence of ectopic pregnancy.
4. Tubal dysplasia: tubal dysplasia or dysfunction can lead to ectopic pregnancy. According to relevant research, female friends of fallopian tube dysplasia, often appear fallopian tube is too long, lack of mucociliary and so on.
5. Multiple artificial abortion: repeated, frequent artificial abortion, will lead to endometrial trauma, embryos are not easy to implantation in the uterine cavity, will be transferred to other places implantation, ectopic pregnancy.
6. Bad habits: long term maintenance of bad living habits will also increase the risk of ectopic pregnancy, for example, smoking, drinking, etc. may increase the incidence of ectopic pregnancy. Another is if female friends often take ovulation induction drugs, etc., will increase the incidence of ectopic pregnancy.
Differential diagnosis of ectopic pregnancy
(1) Urine pregnancy test: simple, fast, positive can help diagnosis, negative need to wait for blood β - hCG quantitative exclusion.
(2) Blood β - hCG quantification: it is an important method for early diagnosis of ectopic pregnancy. It can not only help diagnosis, but also help judge embryo activity to guide treatment. In ectopic pregnancy, serum β - hCG level is usually lower than that of normal intrauterine pregnancy. After conservative drug treatment or surgery, serum β - hCG levels were monitored to detect persistent ectopic pregnancy early.
(3) Serum progesterone determination: the level of progesterone in patients with ectopic pregnancy is low, which can also be used as an indicator for the diagnosis of early ectopic pregnancy. The progesterone level in early pregnancy is relatively stable. For example, progesterone < 45nmol / L (15ng / ml) at 8th week of pregnancy indicates ectopic pregnancy or luteal dysplasia, with a sensitivity of 95%. Serum progesterone levels in normal and abnormal pregnancies overlap, so it is difficult to determine the absolute critical value between them for reference only. Progesterone is listed as a routine monitoring index of ectopic pregnancy in developed countries.
(4) Ultrasound examination: transvaginal ultrasound is superior to abdominal ultrasound in the diagnosis of ectopic pregnancy, the accuracy rate is 70-94%. In order to avoid missed diagnosis of scar pregnancy, it is important to observe the scar position of the anterior wall in patients with history of cesarean section. If the serum β - hCG is more than 2000 mIU / ml, if it is intrauterine pregnancy, vaginal ultrasound can find the gestational sac, otherwise we should be alert to ectopic pregnancy. The fluid dark area of pelvic and abdominal cavity is helpful for diagnosis.
(5) Laparoscopy: is the "gold standard" for the diagnosis of tubal pregnancy, but it is an invasive method with high cost. When the diagnosis is clear, laparoscopic surgery can be carried out at the same time, which avoids the blindness of open surgery, with small trauma and quick recovery. It is widely used in hospitals with conditions. For specific methods, please refer to the chapter "laparoscopy" in this manual.
(6) Endometrial pathological examination: vaginal bleeding is more, ultrasound shows endometrial heterogeneous thickening or with cystic area, diagnostic curettage is feasible, scraping out villi, can be diagnosed as intrauterine pregnancy abortion, otherwise send for pathological examination, if the pathology only see decidua, no villi, it is helpful to diagnose the oocyte transfusion pregnancy. For the ectopic pregnancy with unknown diagnosis, the serum β - hCG can be reexamined 24 hours after curettage. If there is no significant decrease or increase compared with that before operation, the diagnosis is supported. In recent years, with the popularization of assisted pregnancy technology, the incidence of compound pregnancy has increased significantly, so we should pay more attention to it.
Early symptoms of ectopic pregnancy
1. Amenorrhea. Before abortion or rupture of tubal pregnancy, the symptoms and signs were not obvious. In addition to short-term menopause and pregnancy performance, sometimes one side of the lower abdomen distended pain. The fallopian tube was normal or enlarged at the time of examination.
2. Abdominal pain. Lower abdomen drop pain, have defecation feeling, sometimes show intense pain, accompanied by cold sweat dripping. When rupture, the patient suddenly felt tearing pain in one side of the lower abdomen, often accompanied by nausea and vomiting.
3. Other symptoms. The symptoms of ectopic pregnancy are often atypical, some patients will appear nausea, vomiting, frequent urination, urgency, pale face, blood pressure drop and other symptoms.
4. Vaginal bleeding. In the early pregnancy, women may have a small amount of vaginal bleeding, leucorrhea with blood.
5. Syncope and shock. As a result of abdominal acute hemorrhage, can cause blood volume reduction and severe abdominal pain, mild often have syncope, severe shock.
How to do ectopic pregnancy
There are many choices in the treatment of ectopic pregnancy, which depends on the fertility requirements, the size and location of ectopic pregnancy and the physical condition of patients. The fertility of those who have not been given birth should be kept to the maximum extent on the premise of saving the lives of patients.
Drug treatment of ectopic pregnancy
If it is definitely ectopic pregnancy, and the embryo is relatively small, and human chorionic gonadotropin is not very high, the doctor may give you methotrexate (MTX) and other anti-cancer drugs to kill the embryo. Methotrexate is administered intramuscularly, through your blood, to the embryo, which stops ectopic pregnancy by inhibiting cell and placental growth. Over time, this very small embryo can be absorbed by your body. When the drug starts to work, you may feel some abdominal pain or cramps, and you may even have nausea, vomiting and diarrhea. During medication, you should avoid alcohol and sex, and be careful not to take multivitamins or supplements containing folic acid, as these substances can affect the effect of methotrexate.
You also need to go to the hospital for a blood HCG test to see if the embryo of an ectopic pregnancy eventually dies. Because the drug treatment has certain shortcomings: first, in case the drug does not kill the embryo, it will make the embryo longer and bigger, resulting in the rupture of the fallopian tube bleeding. Second, if some embryos are killed and the other part is still alive, old embryos will appear, resulting in female infertility. Therefore, if you have any symptoms of rupture of ectopic pregnancy (such as severe abdominal pain, severe bleeding or shock symptoms) during methotrexate treatment, you need to call 120 at any time.
Surgical treatment of ectopic pregnancy
If you can't use methotrexate under certain circumstances, such as severe pain or abdominal bleeding, or you are breast-feeding, or your health condition does not allow you to use methotrexate, surgery is required for ectopic pregnancy. If your condition is stable and the embryo is small enough, it can be removed by laparoscopy. Through this kind of operation, the doctor puts a miniature camera into your abdominal cavity through a small incision near your navel to observe your fallopian tube. Generally, the embryo or residual tissue can be removed and your fallopian tube can be preserved. However, if the damage to the fallopian tube is serious, or if you have too much bleeding, it may also be removed at the same time.
Laparoscopic surgery requires general anesthesia, special equipment and skilled surgeons, and it takes you about a week to recover. In some cases, for example, if your abdomen has large scar tissue, or bleeding is serious, or the embryo size is too large, it is impossible or not suitable for laparoscopic surgery, then the doctor may do an open surgery for you. When you are anesthetized, the doctor will open your abdomen and take out the embryo. As with laparoscopic surgery, your fallopian tubes may be retained or removed, depending on the circumstances of your operation. After that, you will need about six weeks to recover. During recovery, you may feel some swelling, abdominal pain or other discomfort.